I saw this article for the first time today. Unlike prior articles I have read, this one has specifics on the start of testing.
I saw this article for the first time today. Unlike prior articles I have read, this one has specifics on the start of testing.

When I was trained to use NxStage for home hemodialysis over eight years ago, it required that I always have a trained partner with me while dialyzing. Eventually my wife was getting burned out with the six days per week dialysis.
I researched Respite Care companies and formed a partnership with Helping Hands Respite Care to provide me assistance with dialysis. They were trained by my dialysis nurse and me.
A few months ago the dialysis center offered to train me to run Solo, without any assistance. Based on how long I have been doing home dialysis, the training consisted of running dialysis one day with a nurse watching me dialyze without any assistance.
I have been dialyzing with assistance for so long, and do at times have trouble with low blood pressure, so I was somewhat reluctant to run Solo.
I started Solo by dialyzing on Saturdays with my wife present, but not assisting me. I did this for a couple of weeks and then began running by myself. I have been doing it Solo successfully for over three months.
I sill have occasional low blood pressure episodes, but I control them completely by myself by reducing the amount of water I’m taking off while dialyzing, or occasionally giving myself a saline bolus.
I love the additional freedom this method of dialysis provides by allowing me to adjust the times when I dialyze, and fitting it between my frequent doctor appointments.
I highly recommend that you become trained to run Solo, and start dialyzing this way. I spoke at a home dialysis conference recently, and Fresenius plans to dramatically increase he number of home dialysis patients running solo.
My wife sent me this article a few days ago. As amazing as this seems, trials are to start in 2019, with first patient implants in 2020.
Read the article here – https://forum.facmedicine.com/threads/no-more-dialysis-scientists-have-developed-a-bionic-kidney.28752/
A little over a week ago I started having problems with low or zero pressure readings from my arterial pressure pod. After resetting the pressure pod, within a few minutes I would again have low reading. I attempted to reset it three times. I assumed this was a manufacturing error with the cartridges and begin to just ignore these low readings since I knew my fistula was working great. This continued for five days.
On the sixth day when i was ready to start I pressed run, and immediately got an error 24 – arterial pressure too low. But, I got this error before the pumps had even started. I tried everything I could think of to eliminate this problem, but nothing worked. I called NxStage support and they told me I must have crimped the arterial line when I installed the cartridge. I told them I have been doing this for almost eight years and was very sure I had not crimped the arterial line. I offered maybe I had a bad cartridge. They advised I should setup with a new cartridge and re-prime and it should eliminate this problem.
About an hour later after setting up and priming again I was ready to restart. I got the same error 24 when I pressed run again, before the pumps had even started. Now a second call the MxStage support. A different person assisted me, but was convinced I had a fistula problem. I again told her that I am very experienced with home hemodialysis and I tested my fistula by using an empty syringe to draw out blood from my arterial access, then pushed it back in, and that there was no issue with my fistula. She said I needed to setup a new cartridge a third time and that we would do a mock run to prove whether the issue was with my fistula or the cycler.
I setup again with my now third new cartridge, and re-primed. After I removed all air, I was told to leave all the connections as they were after priming and press run to start the mock run. The mock run would use saline in place of blood to allow the cycler to run like I was being treated. As soon as I pressed run I again I got the error 24. The support person agreed with me that I have a bad cycler and needed a replacement. The new cycler arrived the next day about 3:00 PM and I was back to running like normal.
What I learned from this experience was how to do a mock run. I think this is valuable in determining if you have a cycler problem or a fistula problem.
I also learned to call NxStage technical support for anything unusual that happens. I never called when I was having multiple arterial pressure pod issues because it didn’t prevent me from running. But, it may have assisted NxStage in determining earlier that I was having problems with my cycler, and may have prevented my setting up three different times to diagnose that problem. I don’t know for certain that the arterial pressure pod issues were related to my cycler failure, but since receiving the replacement cycler, I have not had any more pressure pod issues.
As always, I am very impressed with the technical support provided by NxStage and have always been very impressed with how quickly they can provide a replacement cycler.
I have been using NxStage for home hemodialysis for over eight years, and it has become second nature for my wife and I. About a month ago my dialysis center informed me that I would no longer have to complete flow sheets, and that NxStage was providing an automated solution for them.
About a week ago I received a shipment from NxStage and the box contained a new router, a USB pen drive and a wireless device that connects to the cycler Conxbox.
The router requires a high speed Internet connection, and is simply plugged into my existing home router for a access to the Internet. An Ethernet cable was also provided for the connection to my home router.
The USB is used to update the software on the cycler’s ConXbox. It is simply plugged into that device to complete the software update, it took about five minutes. After it is updated, then the wireless device is plugged into any of the USB ports on the ConXbox.
The new iPad was delivered by the dialysis center staff in a few more days. The NxStage iPad has the Nx2me application preloaded, and simply had to connect with the new NxStage router. The application is very easy to use, and automatically records all the details about treatment, including arterial, venus, and effluent pressures.
The application has screens for pre treatment information, a monitor treatment screen for all cycler information while you are dialyzing, and a post treatment screen for entering ending blood pressures, pulse, temperature, ending weight, in addition to many other items related to routine maintenance, labs, etc.
On the monitor treatment screen, there is also the ability to enter notes and medications. One difference I found from using paper flow sheets and the new Nx2me application is recording blood pressures while dialyzing. When using paper flow sheets I took my blood pressure during each 2 halt when the cycler performs checks. The first occurred after 15 minutes, then followed every 32 minutes (2 halts occur after 30 minutes, then 2 more minutes for checks and restart).
The new Nx2me application halts and requests a blood pressure check every 30 minutes, these checks no longer coincide with the 2 halts on the cycler.
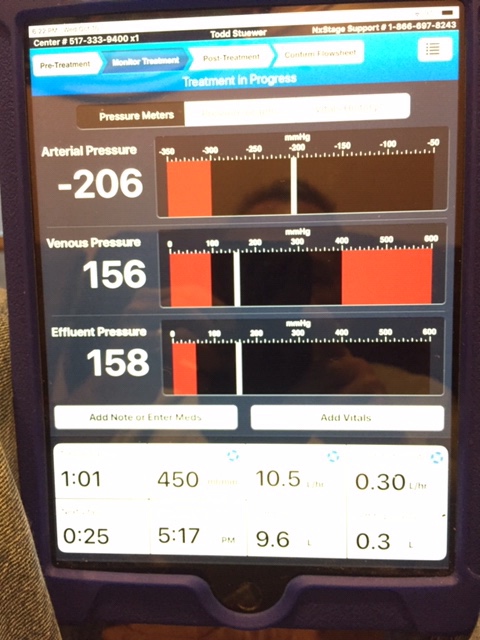
One great improvement is the ability to view all three real time pressures for arterial, venus and effluent. During the times I had issues with either my arterial or venus portions of my fistula, I would have to adjust my needles to lower rising pressures. The cycler only shoes arterial, venus or effluent for a few seconds, then rotates through all the cycler displays. This makes it very difficult to properly adjust a problematic arterial or venus needle. The new Nx2me application shows all three pressures all the time, making this problem much easier to solve.
After using the new application for a few days, I really love the information it provides, it’s ease-of-use and the freedom from completing daily flow sheets and submitting them every month. The new application provides all the details about your dialysis treatment to your local dialysis center within moments of your completion of treatment.
Here a few pictures of the new equipment, and of the Nx2me application screens.
New NxStage router

New wireless device connected to the ConXbox on the cycler

Here is the pre treatment screen
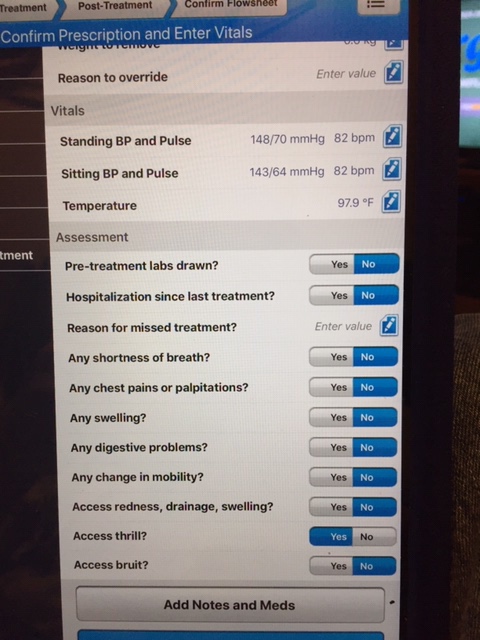
Here is the monitor treatment screen from my last dialysis treatment
And here is the post treatment screen
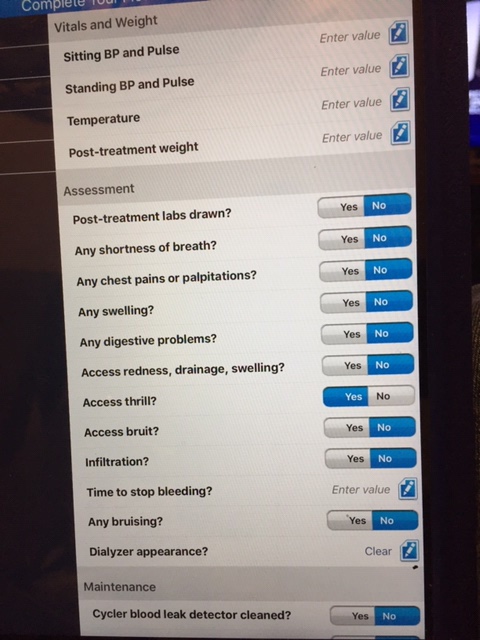
The new application comes with a hardware implementation guide that is easy-to-read and follow. It also include a complete manual for the Nx2me application. This new application will provide more timely information about your dialysis treatments to your dialysis center, your doctor and nurses. It’s easier to use than paper flow sheets and saves me a great deal of time. It’s a really great upgrade, I hope that your dialysis center is providing this to you soon.
When I started in-center hemodialysis over nine years ago, the goal of the dialysis technicians was a pump speed of 500. This allowed the greatest volume of blood to be filtered and cleaned, and provided the highest level of clearance, the amount of cleaning that occurred during treatment.
After numerous trips to the vascular center for clots in my fistula, narrowing and routine semi-annual checkups, the doctor told me frequently that I should lower the pump speed during dialysis from 500 to 450 to help prevent damage to my fistula. I always responded that I have always run at 500, and I didn’t think I should lower my pump speed. Lowering my pump speed would also lengthen the amount of time I spent dialyzing.
I recently had problems with the Venus portion of my fistula, and it became totally unusable. This led to my having to start a new Venus fistula and button-hole (see my blog post https://nxstageusers.wordpress.com/2018/01/07/my-venus-buttonhole-finally-stopped-working-starting-a-new-fistula-and-a-new-venus-buttonhole/ for more details about this).
While forming my new Venus button-hole I had to start with size 17 (much smaller) needles and used a maximum run speed of 200. It took over fours and a half hours to dialyze the first day. The dialysis nurse who helped me with forming the new button-hole told me we could change the setting on my cycler called flow fraction, so that I could raise by dialysate rate, and it would allow me to run for my usual time of just over two hours even running at these extremely low pump speeds.
The next day I changed the cycler setting for flow fraction from 35 to 100. This allowed me to shorten my dialysis time by upping the dialysate rate until my run time showed just over two hours. I now start with a dialysate rate of 7.5, and raise it to 9.5 as I increase the pump speed from my starting speed of 200 to my new maximum of 450.
It’s important that you don’t raise your dialysate rate too high so that you don’t dialyze for at least two hours. If you don’t dialyze for at least two hours, your blood does not get properly cleaned during dialysis. And, the NxStage cycler has to run for a minimum of two hours anyway to remove the volume of water you enter.
Like the arterial physician, my dialysis nurse told me that all the new patients using NxStage use a maximum pump speed of 450. I have been running at 450 now for about two months. I was concerned that even though I use the higher flow fraction and dialysate rate, that I would not get the same high level of clearance that I did while running at pump speed 500.
Yesterday I had my monthly Nephrologist appointment, and my clearance was 2.8, the highest I have ever had. This immediately dispelled my fears that a lower pump speed while dialyzing would lower my blood clearance.
If you were like me, and learned to use NxStage with and continued to use a pump speed of 500, you should consider running at a reduced pump speed of 450 to protect your life-line, your fistula. My run times are now the same as when I ran at 500, and my clearance is even higher than anytime in the past.
About two weeks ago I started having problems getting a good flash with my venus buttonhole access. I normally run at 500, but on a Wednesday, I was unable to run past pump speed 350 due to high Venus pressures.
I visited the Vascular Center on Thursday and they did another angioplasty. I have had numerous procedures for problems with this part of my fistula. I returned home and setup to dialyze that night. Unfortunately, I could not get any flash at all. After trying multiple times I was finally able to get a small flash, and was able to dialyze, but at a very reduced run speed of 350 instead of my usual 500.
The next day my dialysis nurse came to my house and assisted me in using a sharp needle to attempt to start a new buttonhole above my current venus access site. I have a small fistula area, so we had very little room to place a new needle. We were successful two days, but on the following Wednesday I was again unable to run. We assumed there was a clot at the new Venus site.
Another trip to the Vascular Center and another angioplasty to attempt to remove the clot. The doctor felt confident he had removed the clot from the new venus site. The doctor said I also have narrowing in this part of my fistula. That evening, even with my dialysis nurse’s help, we could not get any flash.
The doctor told me during my visit, that I have a “branch” off my regular fistula, and that could be developed and used as a new fistula. We were forced to start using that new “branch” now.
Since I had never used this new location we had to start with small size 17 needle, and use a maximum run speed of 250. My first dialysis session ran over 4 1/2 hours. The next day I changed the flow fraction setting on my NxStage, changing it from 35 to 100. This allowed me to increase my UF rate beyond normal limits to reduce my dialysis time to just over two hours instead of 4 1/2. We used size 17 needles for three more days. Yesterday we went one size larger to size 16 sharp needles, and increased my run speed to 350. After three more days we will then use regular size 15 sharp needles for another three days using a maximum run speed of 450.
On each day the dialysis nurse inserted my sharp needles into the same tract to form my new buttonhole, in addition to developing my new fistula. After the third use of size 16 sharp needles, my new buttonhole will be fully developed and I will then begin using dull buttonhole needles.
A word of warning, do not change the flow fraction on your NxStage cycler without consulting your dialysis center. This setting is set for your personal dialysis needs and should not normally be changed. Mine needed to be changed to both allow me to run faster during fistula development. And, mine will need to ultimately be set at 70 so I can run with a new maximum speed of 450. Running at 450 instead of 500 is easier on your fistula and will help make it last longer.
I feel pretty lucky to have had this additional “branch” on my my fistula. The doctor said normally they would have tied off this extra area, but in my case it had not caused any problems, so the doctor left it as-is.
If I had not had this extra line to be used to form a new fistula, I would have had to go to the hospital and had a catheter inserted in my aorta, then had arterial surgery to create a new fistula, and then had to wait an addition two to three months for it to develop. Catheters can be used in an emergency, but there is also an increased risk of infections with catheters.
Here’s a picture of my new fistula after day three of size 17 sharp needles. Some bruising is normal, and you can clearly see the new fistula is starting to develop even after this short period of use.
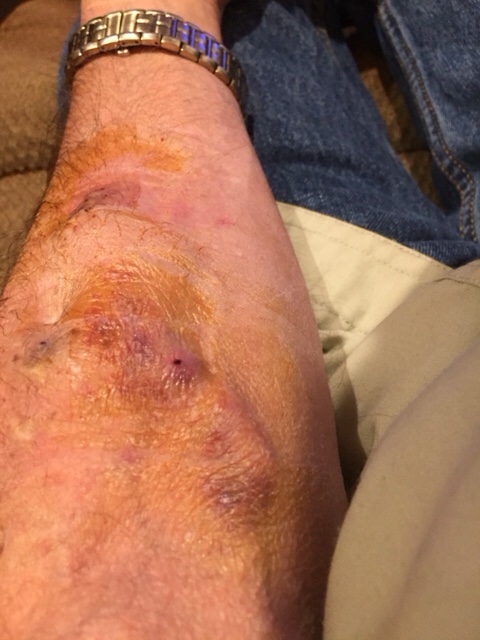
A word of advice, have your fistula checked frequently by a vascular doctor. I have mine checked every six months, and have avoided many problems by doing so. My original fistula has been in use for almost nine years before I had this problem. In another week I’ll have a new venus buttonhole, and will continue to use my original arterial access.
You MUST contact your Congressional Representatives now or you may have to go back to three treatments per week. I received this information from NxStage today via email. Here’s why it matters to you –
A proposed change to Medicare dialysis coverage that could restrict your access to more frequent home hemodialysis.
Here’s what you should know:
• Medicare has a long-standing policy of paying for more frequent hemodialysis treatment when medically necessary and included in a patient’s plan of care.
• Medicare contracts with insurance companies (known as Medicare Administrative Contractors, or “MACs” for short) to manage your Medicare claims and they have the power to determine what qualifies for Medicare coverage and, as a result, what qualifies for Medicare payment.
• Recently, these MACs announced that in most cases, they won’t authorize coverage for more than three hemodialysis sessions per week. If this change happens, Medicare may no longer pay for more than three treatments per week, even if it’s what the doctor wants done.
Here’s how you can help:
•Let your voice be heard TODAY! The MAC that manages your Medicare claims, Medicare and your Members of Congress need to know how important more frequent hemodialysis is to you. As you’ll see below, we’ve worked with the Alliance for Home Dialysis who has a Legislative Action Center where you can quickly and easily get your message to the people who will make the final decision on these proposals.
• This is URGENT. Without an uprising from patients and the entire dialysis community, more frequent dialysis could be denied for thousands of patients as soon as the end of this year. These MACs will soon decide whether these proposed restrictions on more frequent dialysis will happen. Your MAC, Medicare – and your representatives in Congress – need to hear from patients like you about the benefits you have experienced with more frequent hemodialysis. They need to see how this has improved your health and how it makes a difference in your life
• Here’s how to get involved and have your voice heard: It’s easy for you to make a difference and to share your positive experiences with more frequent hemodialysis. Just visit STOPtheMACs.comfor more information about this issue. The website is preloaded with a sample message you can customize and share with your MAC, Medicare and your elected officials with just the click of a button. We’ve even pre-loaded the site with sample messages for you to send on Twitter and Facebook. And please use the hashtag, #STOPtheMACs.
• Help us spread the word to others who care. The MACs and Washington need to hear from people like you – current patients – but also from your friends and loved ones, transplanted patients, caregivers, neighbors, doctors and nurses … anyone who shares our belief that kidney patients should have access to more frequent hemodialysis.
After you send your message, please encourage others to visit STOPtheMACs.com. And don’t forget to use your social media accounts, like Twitter and Facebook, to ask others to help protect patient access to more frequent dialysis. And post a picture or video with your message. Information on how to do that can be found here. And with all of your social media posts, include the hashtag #StoptheMACs.
As you know, more frequent dialysis has significant health benefits, including improved cardiovascular health and blood pressure, reductions in medication requirements, lower overall health care costs, and improvements in post-dialysis recovery time, and quality-of-life. Additional sessions may also increase the chance for transplantation and allow patients to live longer, more productive lives.
Dialysis patients, both now and for years to come, could lose access to more than three treatments per week if the proposed changes are allowed to go into effect.
Now is the time to stand up and make your voice heard, before it’s too late. Please take action today. These MACs will make the decision soon, make certain they’ve heard your voice. If you would like to discuss this issue directly, please contact Linda Upchurch, NxStage Director of Public Policy, at lupchurch@nxsta.com .
Here’s a link to locate you Congressional representatives:
https://www.house.gov/representatives/find/
Here’s a link to contact your Congressional Representatives via Facebook:
https://www.facebook.com/townhall
I used the links above to send my Congressional leaders a note. I followed the recommended text at STOPtheMACS.com, and added another paragraph explains my personal situation, and if this is allowed to continue the drastic negative effect it would have on my life. Please take a few minutes and do the same.
My wife and I have been doing Home Hemodialysis using NxStage for almost seven years.
As a renal failure patient, Home Hemodialysis has dramatically improved my quality of life. I have told my friends and family that my quality of life improved by 100%.
But the wear-and-tear on my wife who assists me almost daily, and continues to work full-time increased every day. Home Hemodialysis for her is like a second job on top of her current full-time job.
We dialyze six times per week, Monday through Friday as soon as she arrives home from work and on a variable schedule on Saturday. I dialyze for just over two hours, and then clean up, so I’m done around 8:30 PM. By the time I made dinner, we wouldn’t eat until 9:00 PM. If we encountered any problems while dialyzing, it might be even later.
My wife eventually said she couldn’t wait until that late to eat dinner, it was affecting her sleep. There is also a great deal of emotional energy expended ensuring there are no mechanical errors, or setup errors I’ve made, or fistula problems, any of which could lead to serious medical consequences, even death.
My wife over the last seven years has assisted me over 2,000 times. But the worst part is her inability to do anything after work. No drinks and conversations with work associates, no educational classes in evenings, she doesn’t even have time to stop for anything on the way home. If I get on Hemodialysis late, I get off even later in the evening.
Her help has been a life-saver for me on multiple occasions, but it dramatically lowered her quality of life being the sole care provider for my serious medical needs on an almost daily basis.
About a year ago, I researched local respite care companies. Most said they do not provide medical care. After further research I located Helping Hands Respite Care and discussed what my wife and I needed. They agreed to investigate providing me with a Home Hemodialysis partner. After many telephone discussions we both decided to move forward with them assisting me on a trial-basis.
My local dialysis provider, Fresenius Medical Care provided four hours of training to two Helping Hands staff. The two staff were very intelligent, dedicated, compassionate and caring.
Both my wife and I had reservations about their ability to take on this responsibility with me, and that some mistakes could be life threatening.
I provided an additional two half days of training, with my wife attending the last training session, and we agreed they are able to handle my needs. I warned Helping Hands management and their two staff that Home Hemodialysis is 2 1/2 hours of sheer boredom, punctuated by occasional moments of sheer terror for both their staff, and for me.
I’ve had NxStage cycler failures while being assisted by Helping Hands, and one time accidentally pulled a needle from my arm, while attempting to adjust my Venus needle to reduce pressure. During both of these incidents, the Helping Hands staff responded calmly, and appropriately, just like my wife would have.
Helping Hands has been assisting me twice per week for almost a year. I consider my partnership with this Respite Care company a great success and am very happy with their services. I also recently joined their Board of Directors.
My wife and I have an improved relationship, she is feeling less stress from Home Hemodialysis, and we now get to eat dinner together two times a week more than we had for many years.
Our relationship was negatively affected by Home Hemodialysis over so many years, but I didn’t realize how hard it is on the care provider. Please do yourself and your partner a favor and discuss this.
If you are lucky enough to live in the Mid-Michigan area, the company I use is willing to assist other NxStage Home Hemodialysis patients:
Helping Hands Respite Care
Jeff Nunham
201 Hillside Court
East Lansing, MI 48910
Ph: (517) 372-6671
http://www.helpinghandsrespite.care/
The most frequently used posts on this blog site are for error 35. Last week after running for 15 minutes I expected to get the first machine stop/check. As soon as it started, I got an error 35, that recurred numerous times.
Unable to clear the error by rinsing the effluent drain line with a syringe, and insuring there were no pinches or kinks in the line, I called NxStage Technical Support. They walked me through multiple procedures in an attempt to diagnose the problem.
One of those was to clamp the two yellow clamps on the effluent line and disconnect the line. Next we put the short line coming from the Pureflow into a bucket and restarted the cycler. This immediately caused another error 35, with the pumps not starting, and nothing coming out of the short effluent line. This proved there was no blockage in the long effluent line that runs to the bathroom and that the problem was in the cycler or the cartridge. If the pump restarted without an error 35 and drained into the bucket, it means there is a blockage in the long line that goes to the drain.
The technician advised that I had a bad cartridge, and that I should do a manual rinse back. We did the manual rinse back, and I would simply set-up again and start over.
After using a new cartridge and setting up, I started treatment and ran normally for three machine stop/checks. Then, just like my previous run I immediately got an error 35, that recurred multiple times, without the pump starting. I called NxStage again, and was walked through numerous steps to determine the problem, and it resulted in needing a replacement cycler.
The final determination of whether an error 35 means you need a replacement cycler is if you get the error 35 immediately after a cycler stop/check, and the errors persists, and the pump never actually starts.